Turning surgery inside out
Richard Downs |
|
 |
|
By KRISTA CONGER
Take it from the ancient Egyptians: Unsightly scarring can be a real drag.
After all, who wants to show up in the afterlife with obvious mummy marks?
But if you think preparing for an eternity of kibitzing with the gods is tricky, just try operating on the face or neck of a prom-bound teenager.
“For children, there is a strong psychological component to having scars,” says pediatric surgeon Sanjeev Dutta, MD. “People tend to think it’s not a big deal and that they should just work through it, but it’s much more complicated than that. The last thing we want to do is to put them at a social disadvantage.” Negative cosmetic side effects can be devastating, confirms Lucile Packard Children’s Hospital pediatric psychologist Michelle Brown, PhD. “As a result, children and adolescents may withdraw from social activities or avoid school for fear of being teased, and their self-esteem may drop if they take to heart the cruel comments made by their peers.”
Egyptian embalmers relied on natural openings such as the nostrils to remove the brain and small abdominal incisions to remove other organs with the least amount of disfigurement. But Dutta has them beat in the creativity department. He and his colleagues at Packard Children’s Hospital use endoscopic surgical tools to remove lesions or perform surgery without obvious scarring by burrowing under the skin from tiny incisions in what until now has been an under-appreciated body part.
Related story: |
|||||
“Finally, armpits have a purpose,” jokes Dutta. “Not only are they a great place to hide surgical scars, but they also provide access to many areas of the body.” Although places like the sides, back, chest, neck and head can be reached from under the arms, few if any pediatric surgeons in the country routinely use them for this purpose, known as subcutaneous endoscopy.
Dutta’s muse was a 7-year-old boy from Guadalajara, Mexico, with torticollis, also known as wryneck. Congenital torticollis can be caused by birth trauma or a uterine position that causes muscles on one side of the neck to contract abnormally. Caught early, it can be treated with gentle, regular neck stretches.
“Unfortunately, this child didn’t have access to appropriate interventions as an infant, and he had developed a significant deformity,” says Dutta. “His eyes had begun to shift position to compensate for his tilted head.” His neck muscle had thickened into a fibrous, inflexible band that needed to be severed to allow normal movement and head position.
But such surgery typically leaves a large scar on the patient’s neck.
Sanjeev Dutta |
|
 |
|
Although Dutta and Packard’s chief of pediatric surgery, Craig Albanese, MD, had previously used a subcutaneous approach to remove a cyst from the forehead of a teen-age girl through incisions hidden in her scalp, reaching the neck from these areas is more difficult. And the surgical entry points can noticeably change hair patterns.
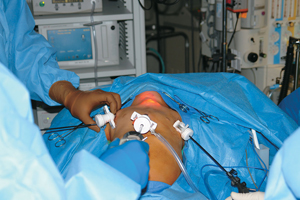
“We were really trying to think about this in a different way,” says Dutta. “The idea evolved from the many types of minimal-access surgery we use to access the abdomen or chest. We wondered if we could create our own cavity under the skin by approaching from below.” Dutta inserted endoscopic tools in three small incisions in the boy’s armpit and threaded them just below the skin up into his neck. After blowing carbon dioxide into the area to make more room to work, he was able to perform the operation without damaging the skin of the boy’s neck.
“We saw the results immediately,” says Dutta. “Although all we did was cut a muscle, we really changed his life. His father was overwhelmed. He had never seen his son hold his head up straight before.”
“This approach is very cool,” says Albanese. “It seems much harder to do than it is, which is probably why nobody else has tried it before. But this will definitely catch on.” All told, the surgeons have performed about 10 subcutaneous procedures, including removing lymph nodes, cysts and other benign lesions.
What’s new under the skin
Although the torticollis case was accomplished through only one armpit, other procedures benefit from using both armpits. The separation allows surgeons to approach the surgical site from either side, giving them more room to maneuver the cutting, grasping, cauterizing and viewing implements. They can also insert tools at the base of the breastbone for a three-pronged approach.
“Endoscopic instruments are basically like long, motorized chopsticks with swappable ends,” says Thomas Krummel, MD, the Emile Holman Professor and chair of surgery at Stanford and the Susan B. Ford Surgeon-in-Chief at Packard. “It’s necessary to have a good angle between them to be effective. Parallel instruments don’t work together very well. It’s very different in an open operation where we can move things around, and our angle and approach are basically unlimited.”
Steve Gladfelter/VAS |
|
 |
|
The subcutaneous layer of the skin is basically loose connective tissue. Threading surgical tools from the incision to the surgical site, though it might seem traumatic, causes no lasting damage as long as major nerves are avoided. Dutta tracks the tools by watching and feeling them move just beneath the skin. The light at the endoscope’s tip also marks its position by shining through the body’s surface. Once in place, the surgeons pump in carbon dioxide to puff up the skin and create a cavity in which to work.
“As we do this more often, we’re learning little tricks,” says Dutta. “Now that we’re more confident with it, we’re fired up to do all sorts of things. This procedure can be used on both adults and kids to address problems all over the body.”
“The surgeons would do every one of their procedures endoscopically if they could. It’s really better for the patients,” says Rosette Reyes, RN, who is responsible for overseeing pediatric general surgery’s nursing operations (the surgeons call her “boss”). “When the surgeons decide to do a new surgery, we go over the whole plan step by step beforehand. Then, when the time comes, we take it really slowly.”
Of course, things aren’t perfect yet. Dutta’s already imagining ways to modify the tools to make the job easier. Although minimal-access surgery makes a surgeon’s job more complicated, the benefits to patients offer great inspiration to develop and master the technique.
“People tend to say that these kids should just tough it out, but they’re not living that child’s life,” says Dutta. “I think that my patients have plenty of time to learn how to be tough later in life.”
Comments? Contact Stanford Medicine at


