A QUICK LOOK at the latest developments from Stanford University Medical Center
![]() A
whole lotta heart
A
whole lotta heart
![]() Young
blood
Young
blood
![]() Radiant
at 100
Radiant
at 100
![]() Diverse
needs
Diverse
needs
![]() You
snooze, you lose
You
snooze, you lose
![]() Cop
doc
Cop
doc
A whole lotta heart
Pound for pound, V. Mohan Reddy’s most remarkable successes don’t add up to much, but their impact has been felt around the world. The cardiovascular surgeon and his colleagues at Lucile Packard Children’s Hospital have made names for themselves by correcting heart defects in newborn babies far too small to undergo the procedures elsewhere.
Gary Taxali |
|
 |
|
“A lot of pediatric cardiologists and neonatologists think these kids are inoperable, but I believe that is a myth,” says Reddy, chief of pediatric cardiac surgery at the hospital and associate professor of cardiothoracic surgery and of pediatrics. “We have the most experience in the world operating on these extremely low birth-weight babies.”
That experience paid off in early February for tiny Jerrick DeLeon, who at 700 grams, or slightly more than 1.5 pounds, became what Reddy believes is the smallest baby ever to survive an open-heart surgery called an arterial switch procedure. The successful operation marked a dramatic turnaround for Jerrick, airlifted to the hospital after doctors in Southern California gave him a zero chance of survival when he was born 13 weeks early with a congenital heart defect.
A grim prognosis
Jerrick needed surgery to correct his condition, known as transposition of the great arteries. However his doctors believed he was too small and premature to undergo the difficult fix, which involves switching the arteries back to their correct positions.
Waiting for Jerrick to grow wasn’t an option; doctors considered it unlikely that he would live long enough to gain the needed weight and strength. But after delivering the grim news to the baby’s parents, his doctors discovered that Reddy had success treating extremely tiny infants. One-week-old Jerrick was airlifted to the hospital on Feb. 4, and Reddy performed the operation two days later.
Happy endings
Jerrick’s successful surgery came three years after Reddy treated Serena Brown, who in 2002 became what is believed to be the smallest baby ever to survive open-heart surgery. She weighed 640 grams, or about the same as two full cans of soda, when Reddy corrected a congenital heart defect in which the veins connecting her lungs to her heart were switched. Serena is now a healthy 3 year old who returns regularly to the hospital for checkups.
Jerrick will likely also be a lifelong fan. After a hard-fought battle with lung problems that afflict many very premature babies, he was released to a hospital closer to his Southern California home. While his medical struggles continue, his heart repair should last his entire — hopefully long — life. His mother, pediatrician Maria Lourdes, MD, couldn’t be more grateful.
“When the pediatrician was telling me about Jerrick’s heart
defect, it just wrecked me emotionally,” she says. “I don’t
know how to express how thankful I am.”— Krista Conger
| ![]() Back
to Top |
Back
to Top |
Young blood
When Tom Rando, MD, PhD, found that muscle stem cells in old muscles are perfectly capable of repairing muscle tissue it begged a question — why don’t they? Why do muscles in older people heal so slowly after an injury?
Gary Taxali |
|
 |
|
He assumed it was something in the older muscle’s environment that kept those stem cells from rescuing damaged muscle. To figure out the cause of the environmental hold-up, Rando, associate professor of neurology and neurological sciences, decided to find out how young blood affects an old mouse. His method: Observe what happens to damaged muscle in an old mouse newly infused with blood from a younger mouse. For the experiment, he connected old and young mice so the two would share a blood supply.
Rando’s studies showed that muscle healed much faster in the older of the joined mice than in unjoined older mice. Furthermore, when old mice were connected to other old mice they healed slowly.
“We need to consider the possibility that the niche in which stem cells sit is as important in terms of stem cell aging as the cells themselves,” says Rando, who is also an investigator at the Veterans Affairs Palo Alto Health Care System. It could be the chemical soup surrounding the cells that’s at fault in aging.
Is it youth serum?
One clue to what might be going on also comes from previous work. Rando had found that stem cells in younger muscles begin producing a protein dubbed Delta in response to muscle damage. Older muscles maintained the same pre-injury levels of Delta even after being damaged. Interestingly, in the current study, published in Nature in February, he found that muscle cells in elderly mice joined to younger partners ramped up Delta production to youthful levels after an injury.
The group confirmed its results by putting muscle stem cells from old and young mice in a lab dish with either old or young blood serum. Old stem cells in old serum and young stem cells in young serum both behaved as expected. But when old muscle stem cells were bathed in young serum they cranked up their production of Delta and began dividing. Likewise, young stem cells decreased the amount of Delta they produced when in a dish with older serum and divided less frequently.
Finding the youth-promoting factors in the blood will be no small task. “It’s as big a fishing expedition as you can possibly imagine,” Rando says. With thousands of proteins, lipids, sugars and other small molecules in the blood serum, deciding where to look first would be tantamount to a roll of the dice. What’s more, there’s no evidence that the same blood component is responsible for reviving different types of cells.
“Another approach is to pick factors that are good candidates
and see if any of them or some combination recapitulate the effect of
the younger blood,” Rando says. His group is now looking for likely
factors in the blood of younger mice. He said that for some degenerative
diseases such as Alzheimer’s or muscular dystrophy, such blood-borne
factors might be able to reactivate the regenerative cells’ ability
to repair damaged tissue. — Amy Adams
| ![]() Back
to Top |
Back
to Top |
Radiant at 100
Ever since Wilhelm Roentgen’s “aha!” moment in 1895, when he stuck his wife’s hand into X-rays and saw her bones illuminated, the technology’s promise for medicine was clear. Nine years later, Stanford University established one of the first radiology departments in the country.
Lane Medical Library
Special Collection & Archives |
|
 |
|
Now 100 years old, the Department of Radiology celebrated its anniversary May 21, standing back and appreciating how much can happen in a century and projecting ahead to the advances of the near future.
Beyond bones
When Stanford hired its first “roentgenologist,” in 1904, he used X-rays to study bones, kidney and gallstones and foreign objects, and to treat skin conditions and cancers. Even at that early stage, X-rays had two very different uses: visualization of internal structures and treatment. Recognizing this divergence, the department eventually split in two in 1986, becoming the Department of Radiology and the Department of Radiation Oncology.
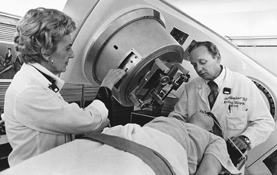
Both branches benefited over the years from collaboration with the campus departments of physics and engineering. Physicists and radiologists combined their skills to develop the nation’s first medical linear accelerator in 1956. Having that equipment led to groundbreaking efforts using radiation therapy to treat Hodgkin’s disease and other lymphomas, as well as a number of other cancers. The present-day incarnation of the early linear accelerators treat more than 100,000 patients a day worldwide.
Gary Glazer, MD, the current chair of the radiology department, says that his father, who was also a radiologist, wouldn’t even recognize, much less comprehend, most radiological equipment in use today. Glazer has seen radiology progress from basic X-rays to the range of imaging possibilities available today, including magnetic resonance imaging, computed tomography, positron emission tomography and ultrasound.
Lane Medical Library
Special Collection & Archives |
|
 |
|
The departments are also celebrating the official opening of a new radiology research facility, completed late last year. The facility, an underground expansion of Stanford’s Lucas Center, houses some of the most advanced MRI equipment in existence, including an 80,000-pound, 7-Tesla whole-body magnet — at 140,000 times the strength of the Earth’s magnetic field, it is one the most powerful MRI magnets in the world — and a high-powered cyclotron to create the radiopharmaceuticals used with a PET scanner.
The vision thing
Despite 100 years of advances in the detection and treatment of diseases such as cancer, Glazer says that “until something fundamentally changes with cancer, the best hope is earlier detection. ” The department’s goals are nothing less than the ability to see individual cancer cells — not the hundreds of billions that it takes to be visualize cancer currently.
This is an advance that will probably occur within the next decade, at least for some cancers. What is beyond that, even the radiologists can’t guess. For example, wonders Glazer, what hidden worlds is the 7T MRI going to illuminate?
“We don’t know yet,” he says. “That’s
what makes it exciting.” — Mitzi Baker
| ![]() Back
to Top |
Back
to Top |
Diverse needs
As a professor of cardiology, Hannah Valantine is a doer by nature. “Cardiology is very much a specialty of intervention; you get in there and you do things,” she says. And her interventional philosophy is readily apparent in her new role as senior associate dean for diversity and leadership at the School of Medicine.
The position was created late last year by Dean Philip Pizzo, MD, who wants the school to do more in attracting women and underrepresented minorities to postgraduate programs and faculty positions.
Valantine, MBBS, MD, says that although the number of women entering the MD, PhD and residency programs continues to increase at Stanford, the growth has been slower at the faculty level. A recent study found that the number of women achieving the rank of professor has hovered around 11 percent for several years. Additionally, the number of minorities entering residency, fellowship and faculty positions has remained flat over the past decade.
John Todd Photography |
|
 |
|
“At the very least, our faculty should represent the proportions of minorities and women in the general population,” says Valantine, who also directs the post-transplant clinical research program.
Although much of her initial focus involves women and minorities, Valantine wants to ensure that all faculty members, regardless of race, gender or sexual orientation, have the support and resources to become leaders in their fields. By mid-April she had already conducted 25 one-on-one meetings with junior faculty to determine what type of support — such as mentorship programs and training in forming effective professional networks — they most want from her office. In addition, she has appointed an executive advisory committee that is working to identify and prioritize the office’s goals for the next three years and map out a strategy to achieve them.
While Valantine hopes to eventually develop a pipeline for recruiting top-notch women and minorities, she first wants to provide support for those already on the faculty. “They have to be our No. 1 focus,” she says.
Another perspective
As a foreign-born black woman working at a U.S. medical school, Valantine has a distinctive viewpoint on diversity and leadership issues. Born in the West African country of Gambia, she moved with her family to England at age 13. When she told her colleagues at London University’s medical school of her interest in cardiology, they were astonished that she was contemplating a specialty dominated by white men.
That attitude has changed over the years, but Valantine says medicine is still a field in which women and minorities feel that their contributions aren’t always valued.
“One of the major missions of the medical school is to build leaders
for the future,” she says. “Everybody is important — and
that includes women and underrepresented minorities.” — Susan
Ipaktchian
| ![]() Back
to Top |
Back
to Top |
You snooze, you lose
Could a few more hours of shut-eye help people shed unwanted pounds? Emmanuel Mignot, MD, PhD, associate professor of psychiatry and behavioral sciences, thinks it might. He recently found that sleep loss leads to higher levels of a hormone that triggers appetite, lower levels of a hormone that tells your body it’s full and more body fat. He’s now gearing up to study whether sleeping more will lead to weight loss.
“Our results demonstrate an important relationship between sleep and metabolic hormones,” Mignot and his co-authors wrote in a paper that appeared in the December 2004 issue of Public Library of Science. “In Western societies, where chronic sleep restriction is common and food is widely available, changes in appetite regulatory hormones with sleep curtailment may contribute to obesity.”
Gary
Taxali |
|
 |
|
Researchers believe that sleep loss impacts several hormones related to appetite and food intake, including ghrelin and leptin. Ghrelin triggers appetite in humans: the more ghrelin you have, the more you want to eat. Leptin is a signal indicating insufficient metabolic reserve and the need for consuming more calories; low leptin levels are a signal for starvation and increased appetite.
While the hormone-sleep connection has been shown under highly controlled laboratory circumstances in past studies, Mignot and his Stanford and University of Wisconsin colleagues wanted to explore the connection in a general population sample.
During the study, the researchers examined the sleep patterns of 1,024 volunteers from a population-based longitudinal study of sleep disorders in Wisconsin. Participants reported on their sleep habits every five years and underwent nocturnal polysomnography and blood sampling once every four years.
The data showed a 14.9 percent increase in ghrelin and a 15.5 percent decrease in leptin in people who consistently slept for five hours compared with those who slept for eight, regardless of participants’ gender, body mass index or eating and exercise habits.
“It was quite amazing that a hormone can track a person’s self-reported amount of sleep so well,” Mignot says. “To my knowledge, this is the first time that a peripheral marker in the blood is shown to correlate with habitual sleep amounts in a general, normally behaving population.”
The researchers also found that in people sleeping less than eight hours, increased BMI was proportional to decreased sleep. They reported that a 3.6 percent increase in BMI corresponded to an average nightly sleep duration decrease from eight hours to five hours.
Encouraged by the results and convinced that more studies are needed, Mignot is now working with a National Institutes of Health researcher to design a sleep administration protocol in chronically sleep-deprived obese subjects. Mignot hopes to begin studying these patients later this year. — Michelle L. Brandt
The National Institutes of Health funded Mignot’s work.
| ![]() Back
to Top |
Back
to Top |
Cop doc
The pitch to Hollywood producers would go like this: Handsome, 40-something director of world-class emergency department who not only wields a scalpel but knows how to fire a gun. Meet the cop doc, a physician who’s ready to tackle any trauma as part of a SWAT — Special Weapons and Tactics — team.
This might sound like some far-out premise for the latest network crime drama, but this one would be reality TV.
Dujuan Green |
|
 |
|
After six months of intensive training at a police academy in San Mateo, Bob Norris, MD, chief of emergency medicine, graduated in March at the top of his class. It isn’t how most professors choose to spend their sabbaticals, but the attacks of Sept. 11, 2001, inspired Norris, 47, to find some way he could thank the law enforcement officers who help to protect the nation.
Norris decided that he wanted to serve as medical support for emergency tactical teams. He began volunteering with the Santa Clara County Sheriff’s tactical medical team a few years ago — the team now has six volunteer medical professionals. Not long after, he and other team members decided to undergo more training in how to conduct themselves in a crime scene.
So in 2003 Norris completed the first tier of training — 180 hours of class and exercises — at the police academy, qualifying to be an entry-level reserve deputy. Still, he wanted the additional training that would allow him to be a full-fledged police officer. That meant doing the six-month program, followed by an internship in the field.
“Extremely challenging” is how Norris describes his latest stint at the academy.
The course runs students through a gauntlet, from a surprise nighttime ambush to a car chase. Recruits can retake any test that they fail, but a second failure means dropping out of the course.
Norris had one close call in an exercise in which he had to search a suspect. He missed a small fork hidden by the suspect’s sleeve. “I went home and told my son that I would pay him $5 for every weapon he hid on his body that I couldn’t find,” he says. Although his son made some good pocket money, Norris passed the test the second time around.
Norris isn’t about to quit his day job to become a police officer. Doing the training is partly for his personal satisfaction. But it’s also helping his work with officers in the field and his research on improving medical care in crime settings.
Norris admits that his sabbatical suprised some of his colleagues. “But after I explain it in the context of tactical medicine and wanting to be a more effective volunteer, they seem to think it makes a lot of sense.” — M.A. Malone
| ![]() Back
to Top |
Back
to Top |
Comments? Contact Stanford Medicine at

