 |
|
Cover Story: Liver Donors take on risks so transplant recipients can survive
By Camille Mojica Rey
Illustration Christian Northeast
Photographs Leslie Williamson
Tom Casey was more than a little relieved when he heard the news on March 18, 2002, that his brother Patrick was well enough to be released from Stanford Hospital. Patrick had endured his body’s attempt to reject the portion of liver Tom had donated to him. “I didn’t realize the rejection had affected me so severely. I didn’t think that I would feel so rejected,” Tom explains. “You just expect: ‘Here. I’ll give you a liver’ and, bam, you’re healed. But you have to let time take its course.” Six weeks after the surgery, doctors had controlled the mild episode of tissue rejection and Patrick’s new liver was functioning well enough so that he could return home to continue his four- to six-month recovery. “It actually helped my recovery knowing he was improving,” Tom says.
Tom’s reaction to Patrick’s improvement underscores the complex nature of the increasingly common procedure of adult-to-adult living liver donation and transplantation. Donors like Tom face financial, physical and emotional challenges, risking their lives in the process. Ensuring the health of the donor adds a level of medical and ethical complexity to a life-or-death situation. Minimizing the risks requires skilled medical professionals, rigorous physical and emotional evaluation of both patients and, as the Casey brothers will tell you, scores of people ready to support both recipient and donor. Scientists have yet to determine the exact risk to donors like Tom. So far, national studies have produced varied results. For the donor, long-term complication rates have been reported to be between 15 and 50 percent, a broad range that begs for more study. The numbers describing the ultimate risk — death — are more straightforward: Of the 1,000 transplants performed in the United States to date, three resulted in the death of the donor.
Despite the risk and complexity, physicians see living donation as at least a temporary solution to the long-term problem of the shortage of liver donors. Helmet, seatbelt and drunk-driving laws in the United States have led to a plateau in the number of cadavers available to supply organs while the U.S. population continues to grow. So while cadaveric livers account for about 5,000 transplants a year, more than 17,500 people were on the waiting list as of April 1, 2002. At the same time, the number of people needing new livers continues to increase as a result of diseases such as Hepatitis C, which is expected to race toward epidemic proportions in this country.
 |
|
Aijaz Ahmed, gastroenterologist, made the diagnosis |
|
One man’s last resort
As Patrick Casey discovered, little-known diseases can destroy one’s liver. He was feeling fine in the spring of 1999 when a routine checkup revealed some abnormalities in the shape of his liver and in subsequent liver function tests. His family physician referred him to Stanford’s Liver Transplant Outreach Clinic in his hometown of Templeton, Calif., north of San Luis Obispo. There he met Aijaz Ahmed, MD, assistant professor of gastroenterology and hepatology, for an initial consultation.
Ahmed later diagnosed Patrick with primary sclerosing cholangitis, or PSC, an autoimmune disease that eventually causes liver failure and, if untreated, death. For Patrick, an active agronomy teacher at the local high school, the diagnosis came as a shock. “I still felt pretty good,” says Patrick, now 50. “I was working out five days a week at the gym.”
The liver is the largest organ in the body and is located in the right upper portion of the abdomen behind the ribs. It stores energy and nutrients, makes vital proteins, metabolizes medications and alcohol, and makes the bile necessary to break down food. In PSC, the body’s immune system mistakenly attacks the bile ducts both inside and outside the liver. This causes inflammation, which leads to scarring, hardening and narrowing of the ducts. Without proper drainage, the bile that normally breaks down food instead damages the liver, leading to the hardening, or cirrhosis, that causes its failure.
By the time Patrick met Ahmed, his liver already showed signs of scarring. “I got extremely sick over the next year,” Patrick recalls. “I just rapidly deteriorated as the disease got worse and worse.” He suffered common symptoms of liver failure, including fluid buildup in his abdomen, extreme weight loss, muscle atrophy and encephalopathy — ammonia accumulation in the brain that slows cognitive function. “It was a continual downward spiral. I couldn’t even say ‘encephalopathy’ when I was sick.”
Patrick’s only hope for recovery was a transplant and he easily qualified to be placed on the national list managed by the United Network for Organ Sharing. But because of Patrick’s critical condition, it became clear to Ahmed that Patrick would not survive long enough to actually receive a liver. That’s when he told Patrick he might consider looking for a living donor.
 |
|
Patrick and Thomas Casey (l. to r.) at Patrick’s home |
|
His brother’s keeper
Tom was among the many people who volunteered, including Patrick’s wife, Denise, and several of their fellow parishioners at Saint Rose of Lima Catholic Church in nearby Paso Robles. “The community really got concerned about my condition and really rallied to help me find a donor.” But, as the youngest and healthiest of Patrick’s four brothers, Tom, 41, turned out to be the best candidate. “Manual labor has kept me pretty fit,” says Tom, who, like his brother, holds a degree in agricultural studies.
The decision to donate was the easiest part, Tom says. “When he called me that night, I said: ‘I’m probably the perfect match for you. I’m your guy.’ ” The evaluation, however, took a lot longer than Tom had expected, requiring him to make frequent trips to Stanford from Clovis, a small town near Fresno. “I think I’ve been tested for just about everything there is,” Tom says. He was evaluated by a cardiologist, a pulmonologist and a hepatologist, among others. “It wasn’t much fun to go through, because I knew Pat was on a timeline. I was getting a bit concerned that I wouldn’t qualify. The longer it took, the weaker my brother was getting.”
An important part of Tom’s assessment was an evaluation by Rae Ann Berry, LCSW, one of the team’s two liver transplant social workers. Berry says her job is to determine if the donor is up to the psychological and emotional challenges of donation. She looks for signs that donors are using their act of giving to fix a troubled relationship or please other family members. “We want to be sure that there’s not any kind of family pressure,” Berry explains. She and the transplant team as a whole also worry about pressure and the more subtle, but equally dangerous, conflict of interest on the part of medical caregivers. To prevent this, one set of doctors, nurses and social workers cares for the donor while a different team cares for the recipient.
Berry ensures that donors have the support they need to get through the evaluation and recovery processes. “It’s not the kind of thing that you can go through alone,” Berry says. Both Tom and Patrick say they had dozens of people each to help cope with daily life while going through this process. Tom says Berry also helped him fill out the paperwork that allowed him to receive disability benefits during the process.
Berry was also instrumental in preparing Tom for what to expect following the surgery. There is more pain for the donor than for the recipient, she points out. “The donors come in perfectly healthy people and then have this huge surgery. Sometimes they are people who haven’t had experience with hospitals or pain. All of it is completely new to them.”
 |
|
Surgeons Maria Millan and Carlos Esquivel |
|
Sharing life
After six months of evaluation, doctors approved Tom Casey as a donor. Professor of surgery Carlos Esquivel, MD, PhD, and assistant professor of surgery Maria Millan, MD, performed the operation on Jan. 28. Esquivel, director of SUMC’s transplant program, was responsible for removing the right lobe of the liver, while Millan transplanted it into Patrick.
Removing so much of a person’s liver is no small feat, Millan says. “It’s a very intricate surgery. The liver is a very vascular organ.” The hardest part for the surgeons, Esquivel agrees, is maintaining the integrity of the lobe. “The technique has to be such that you don’t harm the tissue. The final product has to be a viable lobe.”
If all goes well, both portions of the liver will regenerate to near-normal size within eight weeks of surgery.
Since 2000, the team has performed 14 such operations. The move to adult-to-adult transplants seemed to be a logical one given the experience and expertise of the team that had already been performing adult-to-child operations for more than a decade. The current program relies heavily on existing evaluation protocols and highly skilled specialists. Esquivel, a pioneer in liver transplantation, has participated in nearly 1,500 liver transplant operations. Before coming to Stanford he performed the first transplant involving a recipient under one year old.
Live donation is more feasible for children than for adults because a child needs only about a third of a liver to be saved, explains Esquivel. His team performs about eight living donor transplants a year involving patients at Lucile Packard Children’s Hospital. Moving into adult-to-adult transplantation, where the need is much greater, was the next logical step, Esquivel says.
Right now, the program averages about one adult-to-adult transplant a month. Esquivel would like to see the number double but admits that would require more personnel and resources. As of the beginning of April, five donor/recipient pairs were going through the evaluation process.
 |
|
Rae Ann Berry, social worker on the transplant team |
|
Future of living donation
But because of the risks, Esquivel sees living donation as only a temporary solution. “It’s nerve-wracking to take out so much liver from a healthy person.” One way to ease the demand in the future, he says, is to explore the use of one cadaveric liver to treat two adults: 60 percent of a liver going to an average-sized adult and the remaining 40 percent to a small adult. “That will definitely be our next challenge.”
Cadaveric livers have been successfully shared by an adult and a child. There are, however, far fewer children on the list thanks to donations from parents.
Until there are long-term solutions, Ahmed believes living donation will continue to save the lives of adults. But the procedure will continue to be an option only if strict protocols are followed. In January, a 57-year-old man died at a hospital in New York three days after donating a portion of his liver to his brother. The state fined the hospital $48,000 for inadequate supervision and closed down the living donor liver transplant program for six months.
But as more of these surgeries are performed nationwide, outcomes are likely to improve, Ahmed says. Still, he cautions physicians against becoming complacent. “We should not start to pick marginal candidates,” he explains. “The donors need to be selected cautiously and there should be strict criteria in place.”
 |
|
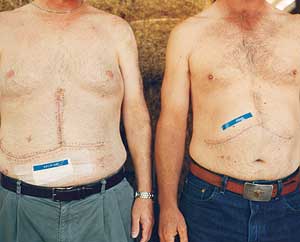
Liver transplant makes its mark on recipient and donor |
|
Despite the risks, both Tom and Patrick Casey are grateful that living liver donation is now an option — and not just because it saved Patrick’s life. Both brothers say they learned to give up their “be-your-own-man” attitudes and let others help them through the ordeal. “It’s an interesting, kind of humbling experience,” Patrick explains. “You realize that you’re not going to get things done by yourself.” The brothers also learned not to take life for granted. As Tom says, “You’re just so glad to be out of the hospital, watching a bird fly by or just driving down the freeway.
“You forget a lot of the simple things until they are taken away from you.”
Comments? Contact Stanford Medicine at

